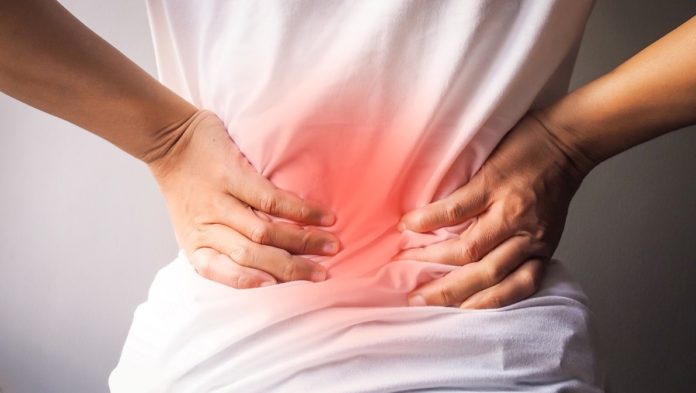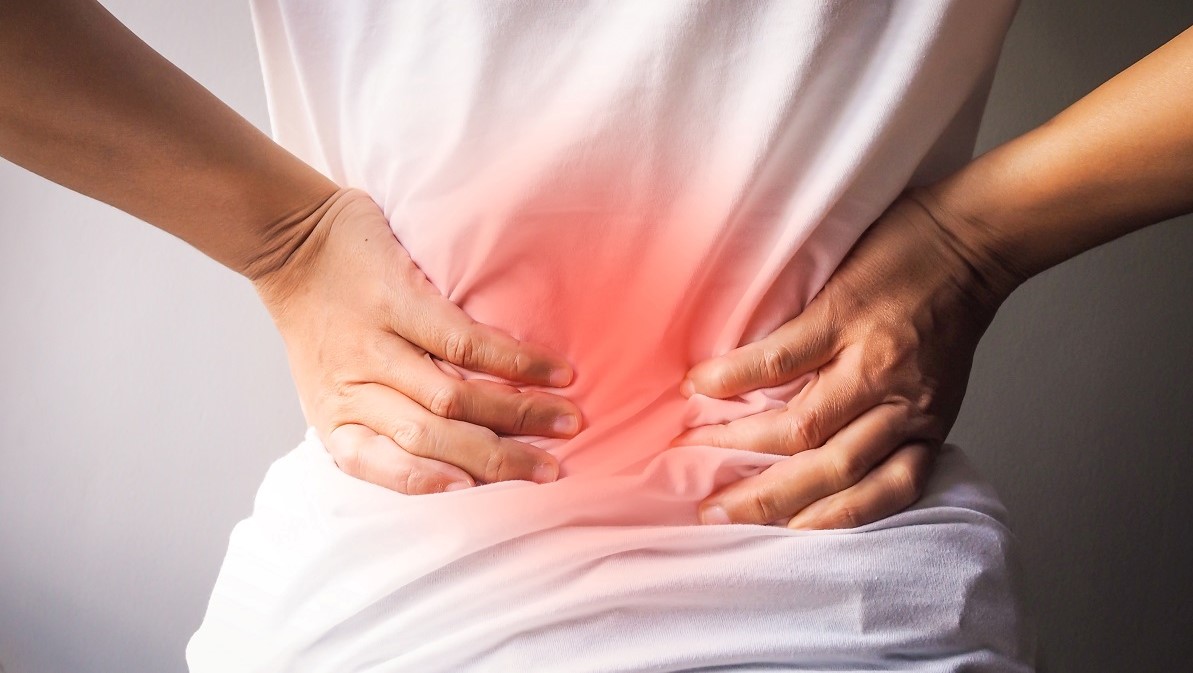
Back pain is a condition that, although generally benign and self-limiting, can condition our day-to-day life, especially if it becomes chronic and becomes disabling.
What is back pain?
Back pain is that which occurs in the back of the trunk, from the occiput to the sacrum.
This denomination also includes painful processes located in areas whose innervation corresponds to the roots or spinal nerves (lumbociatalgia, cervico-brachialgia).
Depending on its duration, back pain is acute (less than 6 weeks), subacute (between 6 weeks and 3 months), chronic (lasts more than 3 months) or recurrent (if successive acute episodes occur, separated by symptom-free periods, of up to 3 months duration).
The problem will be considered to have become chronic when the patient suffers more than three seizures a year.
What are the symptoms of back pain?
Back pain can be:
- Mechanical: it sharpens with movement and decreases or subsides when at rest.
- Inflammatory: does not subside at rest and even reappears or worsens with night rest.
- Neuropathic: pain in the area of injured nerves, which can be described as a sharp tingling with rubbing, and which can radiate to the extremities, with alternating sensation.
As explained by Doctors Ana Victoria Martínez and Rosa Mª Sanchís, from the Quirónsalud Alicante Integral Traumatology Unit, most of the patients who arrive at the consultation do so due to discomfort, of greater or lesser intensity, in the dorsal or lumbar area, usually associated with efforts or bad postures maintained over time. Of all of them, 70% are low back pain.
“The problem, generally, is an overload in the muscles of the dorsolumbar and abdominal trunk that, maintained for a prolonged period, causes discopathies, instabilities and facet osteoarthritis,” they explain. “The most common symptoms described by the patient are discomfort in the lower back, accompanied by pain referred to the buttocks and back of the thigh, and pain radiating to the entire lower limb.”
A visit to the doctor is necessary to control pain or inflammation, although many episodes are brief and limited, and are not serious. In this case, rest, analgesics, or anti-inflammatories may be enough.
However, explain the doctors of Quirónsalud Alicante, there are signs that can alert us to the severity of the pathology. These signs are strength and tenderness disorders, fever, non-postural night pain, or persistence of pain over time.
“The basic test for the diagnosis of a serious back pathology or susceptible to surgery is radiology. Thanks to this, we can locate the exact point of pain, on the one hand, and rule out underlying pathologies, on the other. And, we cannot forget that, sometimes, low back pain can be a symptom of another more serious condition, such as infections, tumours, metastases or gynaecological, urological or abdominal pathology. ”
The difference, according to Drs. Martínez and Sanchís, is that, in this second case, the pain is not mechanical, that is, “it is not related to posture, efforts or standing.”
In this same line, the specialists of the traumatology and spine units can perform an MRI on the patient and “rely on other diagnostic tests such as CT and bone scintigraphy”.
Thanks to them, it is possible to determine what pathology the patient suffers and recommend the most appropriate treatment.
What are the main back pathologies that require surgery?
The main pathologies of the back are:
- Discopathy
- Herniated discs
- Instabilities
- Spondylarthrosis
According to Dr. Juan Antonio Lozano, head of the Spine Unit of Quirónalud Torrevieja, surgery can be recommended to treat both disc pathology manifested by discogenic pain, and lumbar degenerative pathology with involvement of various structures of the vertebral segment (disc, ligament and bone).
Regarding the approach, it will be conditioned by the type of pathology and its severity.
“In case of lumbar disc pathologies without instrumentation, we perform a mini-invasive approach, with a minimum incision, of 3-4 cm.”, explains Dr. Lozano.
“The endoscopic approach, on the other hand, is indicated in lumbar and degenerative foraminal disc pathology without instrumentation and is also little invasive, since the surgery is performed with an incision of 2 cm.”
In case it is necessary to locate implants or make a vertebral fusion, the specialists of Quirónsalud Torrevieja use “percutaneous lumbar instrumentation techniques and surgery with fixation and lumbar arthrodesis, with small incisions of about 2 cm”.
The technique known as lumbar interspinous dynamic fixation is indicated in degenerative pathology in patients of high age or with increased surgical risk. Its advantages are many, since it “reduces surgical time and postoperative recovery, by not performing an instrumented pedicle fusion”.
Postoperative after back surgery
The postoperative period of back surgery depends on the pathology, the surgical technique, and the anatomical region where the surgical procedure has been done.
“In general, anterior cervical pathology has a rapid recovery with little postoperative pain. His hospital stay is about two days,” explains Dr. Lozano.
“Cases of mini-invasive or endoscopic surgery stand out for their rapid functional recovery, with one-day hospital stays. Regarding the techniques of Interspinous Dynamic Fixation in degenerative pathology, they are also well tolerated by most patients, with rapid functional recovery, little pain and hospital stays of about two days”.
The head of the Spine Unit of Quirónsalud Torrevieja, Juan Antonio Lozano, also highlights the importance of preventing back ailments by maintaining a good dorsolumbar and abdominal musculature that helps the spine to transmit loads from our body.
Controlling excess body weight, carefully performing movements such as lifting, pulling, or pushing, in addition to avoiding tobacco, are actions that also contribute to avoiding back pain.
In Quirónsalud we have a team of traumatologists, and neurosurgeons specialised in the diagnosis and surgical treatment of herniated discs and other pathologies of the back.
You can request more information in the traumatology services of Quirónsalud Alicante and Torrevieja